Recognition: 2 theorem links
· Lean TheoremUWB-Fat: Non-Intrusive Body Fat Measurement Using Commodity Ultra-Wideband Radar
Pith reviewed 2026-05-12 00:55 UTC · model grok-4.3
The pith
Ultra-wideband radar measures skinfold thickness to 0.63 mm accuracy without skin contact.
A machine-rendered reading of the paper's core claim, the machinery that carries it, and where it could break.
Core claim
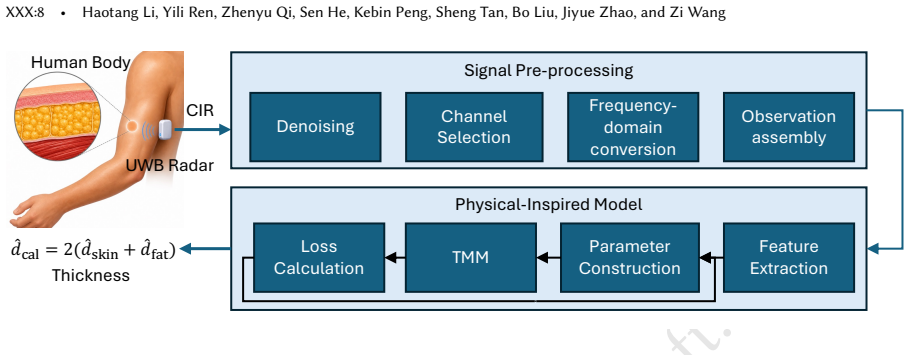
UWB-Fat collects UWB signal at specified body sites non-intrusively without operator assistance. It extracts body-composition-related features from UWB signals by exploiting dielectric contrasts among skin, fat, and muscle tissues. Then, it uses a physics-inspired model to estimate site-specific skinfold thickness. Evaluation on 15 participants yields a root mean square error of 0.63 mm for pooled-site subcutaneous fat thickness.
What carries the argument
Physics-inspired model that converts UWB signal features, derived from dielectric contrasts between skin, fat, and muscle, into site-specific skinfold thickness estimates.
If this is right
- Enables self-administered, contact-free skinfold measurements at multiple body sites using everyday hardware.
- Provides caliper-level accuracy for subcutaneous fat thickness without requiring trained operators or clinical equipment.
- Supports repeated daily or weekly tracking of localized body fat changes at low cost.
- Opens a route to replace intrusive consumer methods such as BIA scales or manual calipers for everyday use.
Where Pith is reading between the lines
- If the approach scales to larger and more varied groups, it could be embedded in consumer devices for continuous personal body-composition monitoring.
- Readings from several sites on the same person might be combined to derive an overall body-fat percentage estimate.
- Individual calibration using a single caliper reading could correct for personal tissue variations and further reduce error.
Load-bearing premise
Dielectric properties of skin, fat, and muscle stay consistent enough across people and conditions that radar reflections map directly to fat thickness without large interference from position, hydration, or other tissues.
What would settle it
A test that shows the thickness estimates deviate by more than 2 mm when the same participant is re-measured after changing posture or drinking water would falsify the claim that the model reliably isolates fat thickness.
Figures




read the original abstract
Body fat percentage and its spatial distribution are clinically important health indicators. However, existing measurement methods often impose a tradeoff between accuracy and accessibility. Clinical-grade techniques, such as Dual-Energy X-ray Absorptiometry (DEXA) and hydrostatic weighing, provide accurate measurements but require specialized equipment and trained operators, making them difficult to access and unsuitable for everyday use. In contrast, consumer-level methods, such as Bioelectrical Impedance Analysis (BIA) smart scales and skinfold calipers, are more accessible but typically provide only coarse-grained estimates, are prone to user error, or require intrusive physical contact. In this work, we present UWB-Fat, the first system that leverages commodity ultra-wideband (UWB) radar to enable non-intrusive, accessible, and accurate caliper-equivalent skinfold thickness estimation, serving as a convenient replacement for the skinfold caliper. UWB-Fat collects UWB signal at specified body sites non-intrusively without operator assistance. It extracts body-composition-related features from UWB signals by exploiting dielectric contrasts among skin, fat, and muscle tissues. Then, it uses a physics-inspired model to estimate site-specific skinfold thickness. We evaluate UWB-Fat on 15 participants, achieving a root mean square error of 0.63~mm for pooled-site subcutaneous fat thickness. These results highlight the potential of UWB-Fat to support low-cost, self-administered, and everyday body fat monitoring.
Editorial analysis
A structured set of objections, weighed in public.
Referee Report
Summary. The paper presents UWB-Fat, a system that uses commodity ultra-wideband (UWB) radar to non-intrusively collect signals at body sites, extracts composition-related features by exploiting dielectric contrasts among skin, fat, and muscle, and applies a physics-inspired model to estimate site-specific subcutaneous fat thickness. It reports a pooled-site RMSE of 0.63 mm versus skinfold calipers on 15 participants and positions the approach as an accessible, contact-free replacement for calipers.
Significance. If the performance and robustness claims hold, the work would provide a meaningful step toward low-cost, self-administered body-composition monitoring that avoids the intrusiveness of calipers or the equipment demands of DEXA/hydrostatic weighing. The emphasis on commodity hardware is a practical strength that could support reproducibility and deployment.
major comments (3)
- [Abstract] Abstract: the headline RMSE of 0.63 mm is presented without any information on participant demographics or selection, the ground-truth caliper protocol (number of sites, operator training, averaging), model derivation details, error bars, or statistical tests. This absence makes the central performance claim impossible to evaluate.
- [Abstract / implied model description] Physics-inspired model (described in abstract and implied methods): the approach relies on fixed dielectric contrasts and a simple reflection geometry to invert for thickness. No equations are supplied, and the evaluation on 15 participants contains no controlled tests for known confounders (hydration, posture, temperature, age-related permittivity variation). If these factors bias the inversion, the reported error is likely optimistic.
- [Evaluation] Evaluation (15-participant study): with a small cohort and no mention of cross-validation, site-specific breakdowns, or leave-one-out analysis, the pooled RMSE cannot be taken as evidence of generalizability across individuals or body sites.
minor comments (2)
- [Abstract] Abstract: the phrase 'pooled-site subcutaneous fat thickness' is ambiguous; clarify whether it aggregates all sites per participant or all measurements across participants.
- [Methods] The manuscript would benefit from an explicit statement of the number of free parameters in the physics-inspired model and how they are obtained (fixed constants versus per-subject fitting).
Simulated Author's Rebuttal
We thank the referee for the constructive and detailed comments, which have helped us improve the clarity and rigor of the manuscript. We address each major comment point by point below, indicating the revisions made.
read point-by-point responses
-
Referee: [Abstract] Abstract: the headline RMSE of 0.63 mm is presented without any information on participant demographics or selection, the ground-truth caliper protocol (number of sites, operator training, averaging), model derivation details, error bars, or statistical tests. This absence makes the central performance claim impossible to evaluate.
Authors: We agree that the abstract requires additional context to allow proper evaluation of the performance claim. In the revised manuscript, we have expanded the abstract to include participant demographics (15 adults aged 20-45 with BMI range 18-32), the caliper protocol (three standard sites per participant measured by a trained operator with three repetitions averaged per site), and a brief note on error bars and correlation with ground truth. Model derivation details remain in Section 3 due to abstract length constraints, but we now reference them explicitly. revision: yes
-
Referee: [Abstract / implied model description] Physics-inspired model (described in abstract and implied methods): the approach relies on fixed dielectric contrasts and a simple reflection geometry to invert for thickness. No equations are supplied, and the evaluation on 15 participants contains no controlled tests for known confounders (hydration, posture, temperature, age-related permittivity variation). If these factors bias the inversion, the reported error is likely optimistic.
Authors: We acknowledge that the original manuscript did not present the explicit equations for the multi-layer reflection model. In the revision, we have added the full equations in Section 3.2, including the reflection coefficient formula and inversion for fat thickness based on literature-derived dielectric constants. Regarding confounders, we have added a dedicated Limitations subsection discussing hydration, posture, temperature, and age-related permittivity effects. The study was performed under standardized conditions, but we agree no systematic controlled variation was conducted; we now explicitly state that this may render the reported error optimistic and outline plans for future validation. revision: yes
-
Referee: [Evaluation] Evaluation (15-participant study): with a small cohort and no mention of cross-validation, site-specific breakdowns, or leave-one-out analysis, the pooled RMSE cannot be taken as evidence of generalizability across individuals or body sites.
Authors: We agree that the small cohort and lack of additional analyses limit claims of generalizability. In the revised manuscript, we have added site-specific RMSE values (ranging 0.48-0.79 mm across triceps, abdomen, and thigh) in Table 2 and performed leave-one-subject-out cross-validation, reporting a mean RMSE of 0.71 mm (std 0.14 mm). These results are now presented in Section 4.3. We have also revised the discussion to temper claims of generalizability and emphasize the preliminary nature of the 15-participant evaluation. revision: yes
Circularity Check
No significant circularity; physics model uses external dielectric constants with empirical validation
full rationale
The provided abstract and context describe a physics-inspired model that exploits known dielectric contrasts among skin, fat, and muscle to estimate skinfold thickness from UWB signals, followed by direct evaluation against caliper measurements on 15 participants (RMSE 0.63 mm). No equations, fitting procedures, or self-citations are quoted that would make the thickness output equivalent to its inputs by construction, rename a fitted parameter as a prediction, or rely on author-overlapping uniqueness theorems. The derivation chain remains self-contained against external physical constants and independent ground-truth data.
Axiom & Free-Parameter Ledger
free parameters (1)
- model coefficients for dielectric contrast mapping
axioms (1)
- domain assumption Dielectric constants of skin, fat, and muscle are sufficiently distinct and stable to produce distinguishable UWB reflections at the frequencies used
Lean theorems connected to this paper
-
IndisputableMonolith/Cost/FunctionalEquation.leanwashburn_uniqueness_aczel unclear?
unclearRelation between the paper passage and the cited Recognition theorem.
We model this anatomy as a stratified tissue stack comprising a skin layer of thickness ds, a fat layer of thickness df, and a muscle half-space... Fresnel reflection coefficient Γn(f) at the interface... Transfer-Matrix Method... M = M0P M01I M1P M12I M2P M23I
-
IndisputableMonolith/Foundation/AbsoluteFloorClosure.leanreality_from_one_distinction unclear?
unclearRelation between the paper passage and the cited Recognition theorem.
the physics-inspired model... jointly recovers skin thickness, fat thickness, and the antenna-skin air gap by minimizing the broadband data misfit against the closed-form layered-tissue forward model
What do these tags mean?
- matches
- The paper's claim is directly supported by a theorem in the formal canon.
- supports
- The theorem supports part of the paper's argument, but the paper may add assumptions or extra steps.
- extends
- The paper goes beyond the formal theorem; the theorem is a base layer rather than the whole result.
- uses
- The paper appears to rely on the theorem as machinery.
- contradicts
- The paper's claim conflicts with a theorem or certificate in the canon.
- unclear
- Pith found a possible connection, but the passage is too broad, indirect, or ambiguous to say the theorem truly supports the claim.
Reference graph
Works this paper leans on
-
[1]
Fadel Adib, Hongzi Mao, Zachary Kabelac, Dina Katabi, and Robert C. Miller. 2015. Smart Homes that Monitor Breathing and Heart Rate. InProceedings of the 33rd Annual ACM Conference on Human Factors in Computing Systems(Seoul, Republic of Korea)(CHI ’15). Association for Computing Machinery, New York, NY, USA, 837–846. doi:10.1145/2702123.2702200
-
[2]
S. Agrawal, M. D. R. Klarqvist, N. Diamant, T. L. Stanley, P. T. Ellinor, N. N. Mehta, A. Philippakis, K. Ng, M. Claussnitzer, S. K. Grinspoon, P. Batra, and A. V. Khera. 2023. BMI-adjusted adipose tissue volumes exhibit depot-specific and divergent associations with cardiometabolic diseases.Nat Commun14, 1 (2023), 266. doi:10.1038/s41467-022-35704-5
-
[3]
Terence W Barrett. 2001. History of ultra wideband communications and radar: part I, UWB communications.Microwave Journal44, 1 (2001), 22–56. Unpublished working draft.Not for distribution. UWB-Fat: Non-Intrusive Body Fat Measurement Using Commodity Ultra-Wideband Radar•XXX:23
work page 2001
-
[4]
Thomas Baum, Christian Cordes, Michael Dieckmeyer, Stefan Ruschke, Daniela Franz, Hans Hauner, Jan S Kirschke, and Dimitrios C Karampinos. 2016. MR-based assessment of body fat distribution and characteristics.European Journal of Radiology85, 8 (2016), 1512–1518
work page 2016
-
[5]
J Martin Bland and Douglas G Altman. 1986. Statistical methods for assessing agreement between two methods of clinical measurement. The Lancet327, 8476 (1986), 307–310
work page 1986
-
[6]
Yifeng Cao, Ashutosh Dhekne, and Mostafa Ammar. 2024. UWB-Auth: A UWB-based Two Factor Authentication Platform. InProceedings of the 17th ACM Conference on Security and Privacy in Wireless and Mobile Networks(Seoul, Republic of Korea)(WiSec ’24). Association for Computing Machinery, New York, NY, USA, 185–195. doi:10.1145/3643833.3656113
-
[7]
Mohammad Cheraghinia, Adnan Shahid, Stijn Luchie, Gert-Jan Gordebeke, Olivier Caytan, Jaron Fontaine, Ben Van Herbruggen, Sam Lemey, and Eli De Poorter. 2024. A comprehensive overview on UWB radar: Applications, standards, signal processing techniques, datasets, radio chips, trends and future research directions.IEEE Communications Surveys & Tutorials27, ...
work page 2024
-
[8]
Ivana Čuljak, Željka Lučev Vasić, Hrvoje Mihaldinec, and Hrvoje Džapo. 2020. Wireless body sensor communication systems based on UWB and IBC technologies: State-of-the-art and open challenges.Sensors20, 12 (2020), 3587
work page 2020
-
[9]
Mahshid Dehghan and Anwar T Merchant. 2008. Is bioelectrical impedance accurate for use in large epidemiological studies?Nutrition Journal7 (2008), 26. doi:10.1186/1475-2891-7-26
-
[10]
Ellen W Demerath, SS Guo, WC Chumlea, B Towne, AF Roche, and RM Siervogel. 2002. Comparison of percent body fat estimates using air displacement plethysmography and hydrodensitometry in adults and children.International journal of obesity26, 3 (2002), 389–397
work page 2002
-
[11]
Nathan DeVrio, Vimal Mollyn, and Chris Harrison. 2023. SmartPoser: Arm Pose Estimation with a Smartphone and Smartwatch Using UWB and IMU Data. InProceedings of the 36th Annual ACM Symposium on User Interface Software and Technology(San Francisco, CA, USA)(UIST ’23). Association for Computing Machinery, New York, NY, USA, Article 79, 11 pages. doi:10.1145...
-
[12]
Cailbhe Doherty, Maximus Baldwin, Rory Lambe, Marco Altini, and Brian Caulfield. 2025. Privacy in consumer wearable technologies: a living systematic analysis of data policies across leading manufacturers.npj Digital Medicine8, 1 (2025), 363. doi:10.1038/s41746-025- 01757-1
-
[13]
J. V. G. A. Durnin and J. Womersley. 1974. Body fat assessed from total body density and its estimation from skinfold thickness: measurements on 481 men and women aged from 16 to 72 years.British Journal of Nutrition32, 1 (1974), 77–97
work page 1974
-
[14]
David A Fields, Michael I Goran, and Megan A McCrory. 2002. Body-composition assessment via air-displacement plethysmography in adults and children: a review.The American Journal of Clinical Nutrition75, 3 (2002), 453–467. doi:10.1093/ajcn/75.3.453
-
[15]
S Gabriel, R W Lau, and Camelia Gabriel. 1996. The dielectric properties of biological tissues: II. Measurements in the frequency range 10 Hz to 20 GHz.Physics in Medicine and Biology41, 11 (1996), 2251–2269
work page 1996
-
[16]
Akram Gasmelseed. 2025. Parametric analysis of electromagnetic wave interactions with layered biological tissues for varying frequency, polarization, and fat thickness.Scientific Reports16, 1 (2025), 3445. doi:10.1038/s41598-025-33460-2
-
[17]
Walter O Grauer, Albert A Moss, Christopher E Cann, and Henry I Goldberg. 1984. Quantification of body fat distribution in the abdomen using computed tomography.The American journal of clinical nutrition39, 4 (1984), 631–637
work page 1984
-
[18]
Hany, Hamada Rizk, and Moustafa Youssef
Mohamed I. Hany, Hamada Rizk, and Moustafa Youssef. 2024. AirTags for Human Localization, Not Just Objects. InProceedings of the 2nd ACM SIGSPATIAL International Workshop on Geo-Privacy and Data Utility for Smart Societies(Atlanta, GA, USA)(GeoPrivacy ’24). Association for Computing Machinery, New York, NY, USA, 13–18. doi:10.1145/3681768.3698497
-
[19]
P A Hasgall, F Di Gennaro, C Baumgartner, E Neufeld, B Lloyd, M C Gosselin, D Payne, A Klingenböck, and N Kuster. 2022. IT’IS Database for thermal and electromagnetic parameters of biological tissues, Version 4.1. doi:10.13099/VIP21000-04-1
- [20]
-
[21]
Steven B. Heymsfield. 2025. Advances in body composition: a 100-year journey.International Journal of Obesity49, 2 (2025), 177–181. doi:10.1038/s41366-024-01511-9 Published online 2024; print 2025
-
[22]
Chen-Yu Hsu, Yuchen Liu, Zachary Kabelac, Rumen Hristov, Dina Katabi, and Christine Liu. 2017. Extracting Gait Velocity and Stride Length from Surrounding Radio Signals. InProceedings of the 2017 CHI Conference on Human Factors in Computing Systems(Denver, Colorado, USA)(CHI ’17). Association for Computing Machinery, New York, NY, USA, 2116–2126. doi:10.1...
-
[23]
Andrew S Jackson and Michael L Pollock. 1978. Generalized equations for predicting body density of men.British Journal of Nutrition 40, 3 (1978), 497–504. doi:10.1079/BJN19780152
-
[24]
A. S. Jackson, M. L. Pollock, and A. Ward. 1980. Generalized equations for predicting body density of women.Medicine and Science in Sports and Exercise12, 3 (1980), 175–181
work page 1980
-
[25]
Ahmad Jayedi, Tauseef Ahmad Khan, Dagfinn Aune, Alireza Emadi, and Sakineh Shab-Bidar. 2022. Body fat and risk of all-cause mortality: a systematic review and dose-response meta-analysis of prospective cohort studies.International Journal of Obesity46, 9 (2022), 1573–1581. doi:10.1038/s41366-022-01165-5
-
[26]
Suk Hwa Jung, Kyoung Hwa Ha, and Dae Jung Kim. 2016. Visceral Fat Mass Has Stronger Associations with Diabetes and Prediabetes than Other Anthropometric Obesity Indicators among Korean Adults.Yonsei Medical Journal57, 3 (2016), 674–680. doi:10.3349/ymj. 2016.57.3.674 Unpublished working draft.Not for distribution. XXX:24•Haotang Li, Yili Ren, Zhenyu Qi, S...
work page doi:10.3349/ymj 2016
-
[27]
Karvonen, Noboru Kimura, and Henry L
Ancel Keys, Flaminio Fidanza, Martti J. Karvonen, Noboru Kimura, and Henry L. Taylor. 1972. Indices of relative weight and obesity. Journal of Chronic Diseases25, 6 (1972), 329–343. doi:10.1016/0021-9681(72)90027-6
-
[28]
Young Jae Kim, Seung Hyun Lee, Tae Yun Kim, Jeong Yun Park, Seung Hong Choi, and Kwang Gi Kim. 2013. Body fat assessment method using CT images with separation mask algorithm.Journal of digital imaging26, 2 (2013), 155–162
work page 2013
-
[29]
Maciej Klemm, Ian J Craddock, Jack A Leendertz, Alan Preece, and Ralph Benjamin. 2009. Radar-based breast cancer detection using a hemispherical antenna array: experimental results.IEEE Transactions on Antennas and Propagation57, 6 (2009), 1692–1704. doi:10.1109/TAP.2009.2019856
-
[30]
Jennifer R Kwapisz, Gary M Weiss, and Samuel A Moore. 2011. Activity recognition using cell phone accelerometers.ACM SIGKDD Explorations Newsletter12, 2 (2011), 74–82. doi:10.1145/1964897.1964918
-
[31]
Ursula G Kyle, Ingvar Bosaeus, Antonio D De Lorenzo, Paul Deurenberg, Marinos Elia, Jose Manuel Gómez, Berit Lilienthal Heitmann, Lisa Kent-Smith, Jean-Claude Melchior, Matthias Pirlich, et al. 2004. Bioelectrical impedance analysis—part I: review of principles and methods.Clinical Nutrition23, 5 (2004), 1226–1243
work page 2004
-
[32]
Mariya Lazebnik, Dijana Popovic, Leah McCartney, et al. 2007. A large-scale study of the ultrawideband microwave dielectric properties of normal, benign and malignant breast tissues obtained from cancer surgeries.Physics in Medicine & Biology52, 20 (2007), 6093–6115. doi:10.1088/0031-9155/52/20/002
-
[33]
Deanna K Levenhagen, Myfanwy J Borel, Derek C Welch, Justin H Piasecki, Dana P Piasecki, Kong Y Chen, and Paul J Flakoll. 1999. A comparison of air displacement plethysmography with three other techniques to determine body fat in healthy adults.Journal of Parenteral and Enteral Nutrition23, 5 (1999), 293–299
work page 1999
-
[34]
Jaime Lien, Nicholas Gillian, M Emre Karagozler, Patrick Amihood, Carsten Schwesig, Erik Olson, Hakim Raja, and Ivan Poupyrev
-
[35]
Soli: ubiquitous gesture sensing with millimeter wave radar.ACM Transactions on Graphics35, 4, Article 142 (2016), 19 pages. doi:10.1145/2897824.2925953
-
[36]
Dalmo Roberto Lopes Machado, Leonardo Santos Lopes da Silva, Raquel Vaquero-Cristóbal, Victor Carvalheiro Rosa, Marcio Fer- nando Tasinafo Junior, André Pereira dos Santos, Pedro Pugliesi Abdalla, Lisa Fernanda Mazzonetto, Alcivandro Sousa de Oliveira, Jorge Mota, and Pablo Jorge Marcos-Pardo. 2025. Reliability of skinfold measurements and body fat predic...
-
[37]
Marko Malajner, Peter Planinšič, and Dušan Gleich. 2015. UWB ranging accuracy. In2015 International Conference on Systems, Signals and Image Processing (IWSSIP). IEEE, London, UK, 61–64. doi:10.1109/IWSSIP.2015.7314177
-
[38]
K N Manolopoulos, F Karpe, and K N Frayn. 2010. Gluteofemoral body fat as a determinant of metabolic health.International Journal of Obesity34, 6 (2010), 949–959. doi:10.1038/ijo.2009.286
-
[39]
Carmelo Messina, Domenico Albano, Salvatore Gitto, Laura Tofanelli, Alberto Bazzocchi, Fabio Massimo Ulivieri, Giuseppe Guglielmi, and Luca Maria Sconfienza. 2020. Body composition with dual energy X-ray absorptiometry: from basics to new tools.Quantitative Imaging in Medicine and Surgery10, 8 (2020), 1687–1698. doi:10.21037/qims.2020.03.02
-
[40]
Daniel Minoli and Benedict Occhiogrosso. 2018. Ultrawideband (UWB) Technology For Smart Cities IoT Applications. In2018 IEEE International Smart Cities Conference (ISC2). IEEE, Kansas City, MO, USA, 1–8. doi:10.1109/ISC2.2018.8656958
-
[41]
Puyan Mojabi and Joe LoVetri. 2009. Overview and classification of some regularization techniques for the Gauss-Newton inversion method applied to inverse scattering problems.IEEE Transactions on Antennas and Propagation57, 9 (2009), 2658–2665. doi:10.1109/TAP. 2009.2027161
work page doi:10.1109/tap 2009
-
[42]
Ramakrishna Mukkamala, Jin-Oh Hahn, Omer T Inan, Lalit K Mestha, Chang-Sei Kim, Hakan Töreyin, and Survi Kyal. 2015. Toward ubiquitous blood pressure monitoring via pulse transit time: theory and practice.IEEE Transactions on Biomedical Engineering62, 8 (2015), 1879–1901. doi:10.1109/TBME.2015.2441951
-
[43]
Hans-Peter Müller, Florian Raudies, Alexander Unrath, Heiko Neumann, Albert C Ludolph, and Jan Kassubek. 2011. Quantification of human body fat tissue percentage by MRI.NMR in Biomedicine24, 1 (2011), 17–24
work page 2011
-
[44]
Novelda AS. 2024. X7F202 Ultra-Wideband Impulse Radar Transceiver SoC: Advance Datasheet, Rev. 3.0. Datasheet. 750 MHz TX -10 dB bandwidth, 7.875 GHz center frequency, 2100 MS/s sampling
work page 2024
-
[45]
Sameera Palipana, David Rojas, Piyush Agrawal, and Dirk Pesch. 2018. FallDeFi: Ubiquitous Fall Detection using Commodity Wi- Fi Devices.Proceedings of the ACM on Interactive, Mobile, Wearable and Ubiquitous Technologies1, 4, Article 155 (2018), 25 pages. doi:10.1145/3161183
-
[46]
1993.High-Performance Bodybuilding
John Parrillo and Maggie Greenwood-Robinson. 1993.High-Performance Bodybuilding. Perigee Trade, New York
work page 1993
-
[47]
R. Gerhard Pratt. 1999. Seismic waveform inversion in the frequency domain, Part 1: Theory and verification in a physical scale model. Geophysics64, 3 (1999), 888–901. doi:10.1190/1.1444597
-
[48]
Andrew M Prentice and Susan A Jebb. 2001. Beyond body mass index.Obesity Reviews2, 3 (2001), 141–147. doi:10.1046/j.1467- 789x.2001.00031.x
-
[49]
Meaney, Peter Meincke, and Keith D
Tonny Rubæk, Paul M. Meaney, Peter Meincke, and Keith D. Paulsen. 2007. Nonlinear microwave imaging for breast-cancer screening using Gauss-Newton’s method and the CGLS inversion algorithm.IEEE Transactions on Antennas and Propagation55, 8 (2007), 2320–2331. Unpublished working draft.Not for distribution. UWB-Fat: Non-Intrusive Body Fat Measurement Using ...
-
[50]
Mariella Särestöniemi. 2020.UWB in-body propagation and radio channel characteristics for wireless body area network applications. Ph. D. Dissertation. University of Oulu
work page 2020
-
[51]
Wei Shen, ZiMian Wang, Mark Punyanita, Jianbo Lei, Ahmet Sinav, John G Kral, Celina Imielinska, Robert Ross, and Steven B Heymsfield. 2003. Adipose tissue quantification by imaging methods: a proposed classification.Obesity Research11, 1 (2003), 5–16. doi:10.1038/oby.2003.3
-
[52]
Courtney C. Simpson and Suzanne E. Mazzeo. 2017. Calorie counting and fitness tracking technology: Associations with eating disorder symptomatology.Eating Behaviors26 (2017), 89–92. doi:10.1016/j.eatbeh.2017.02.002
-
[53]
L Sjostrom, H Kvist, A Cederblad, and U Tylen. 1986. Determination of total adipose tissue and body fat in women by computed tomography, 40K, and tritium.American Journal of Physiology-Endocrinology And Metabolism250, 6 (1986), E736–E745
work page 1986
-
[54]
M. H. Slaughter, T. G. Lohman, R. A. Boileau, C. A. Horswill, R. J. Stillman, M. D. Van Loan, and D. A. Bemben. 1988. Skinfold equations for estimation of body fatness in children and youth.Human Biology60, 5 (1988), 709–723
work page 1988
-
[55]
A. Stewart, M. Marfell-Jones, T. Olds, and H. de Ridder. 2011.International Standards for Anthropometric Assessment. International Society for the Advancement of Kinanthropometry (ISAK), Lower Hutt, New Zealand
work page 2011
-
[56]
Robert Streeter, Jooeun Lee, Gabriel Santamaria Botello, and Zorana Popović. 2024. Classification of multi-layer tissue-mimicking dielectric stacks from 2 to 20 GHz.IEEE Journal of Electromagnetics, RF and Microwaves in Medicine and Biology9, 1 (2024), 36–41
work page 2024
-
[57]
Albert Tarantola. 1984. Inversion of seismic reflection data in the acoustic approximation.Geophysics49, 8 (1984), 1259–1266. doi:10.1190/1.1441754
-
[58]
James D. Taylor (Ed.). 2001.Ultra-Wideband Radar Technology. CRC Press, Boca Raton, FL
work page 2001
-
[59]
James D. Taylor. 2012.Ultrawideband Radar: Applications and Design(1st ed.). CRC Press, Inc., USA
work page 2012
-
[60]
André Tchernof and Jean-Pierre Després. 2013. Pathophysiology of human visceral obesity: an update.Physiological Reviews93, 1 (2013), 359–404. doi:10.1152/physrev.00033.2011
-
[61]
E Louise Thomas, Nadeem Saeed, Joseph V Hajnal, Audrey Brynes, Anthony P Goldstone, Gary Frost, and Jimmy D Bell. 1998. Magnetic resonance imaging of total body fat.Journal of applied physiology85, 5 (1998), 1778–1785
work page 1998
-
[62]
Henk Wymeersch, Stefano Maranò, Wesley M Gifford, and Moe Z Win. 2012. A machine learning approach to ranging error mitigation for UWB localization.IEEE transactions on communications60, 6 (2012), 1719–1728
work page 2012
-
[63]
M.S. Yuhasz. 1974.Physical Fitness Manual. University of Western Ontario, London, Ontario. https://books.google.com/books?id= oPgMtwAACAAJ
work page 1974
-
[64]
Roberta de Vargas Zanini, Iná S Santos, Maria Aurora D Chrestani, and Denise Petrucci Gigante. 2015. Body fat in children measured by DXA, air-displacement plethysmography, TBW and multicomponent models: a systematic review.Maternal and child health journal19, 7 (2015), 1567–1573
work page 2015
-
[65]
H. Zhou, T. Li, J. Li, et al. 2024. The association between visceral adiposity index and risk of type 2 diabetes mellitus.Scientific Reports 14 (2024), 16634. doi:10.1038/s41598-024-67430-x
-
[66]
Lukasz Zwirello, Tom Schipper, Marlene Harter, and Thomas Zwick. 2012. UWB localization system for indoor applications: Concept, realization and analysis.Journal of Electrical and Computer Engineering2012, 1 (2012), 849638
work page 2012
discussion (0)
Sign in with ORCID, Apple, or X to comment. Anyone can read and Pith papers without signing in.